As a runner, consider this all-too-familiar situation:
Halfway into a run, you feel a gradual ache begin to develop somewhere in one of your legs. Often, we runners tell ourselves, “It will go away in the next mile or two.” And so, we keep running. But after two more (annoying) miles, the ache persists. Even more concerning, the ache does not go away for the entire run. Worst case scenario: it lasts the rest of the day and into the next day too! Now, many questions flood our minds about what this ache is, what it means for our training, and what it may do to our running goals. Read on to learn how to answer and calm your racing thoughts, how to differentiate soreness from pain, and if you can keep running with these symptoms. (Hint: you may be surprised by our answer!)
Soreness
Typically, soreness is a shortened term for “Delayed Onset Muscle Soreness” (DOMS) which can feel like tired, achy, or stiff muscles and joints. Sometimes this muscle soreness occurs right after a workout. Other times, DOMS can take up to 24-48 hours after a workout to appear. DOMS can last up to 72 hours after the workout’s completion too. DOMS is more likely to occur when the training increases from a previous level or when the workout focuses more on eccentric muscle contractions (i.e., negatives in weight lifting or running downhill).The main cause of DOMS involves microtrauma to the muscles that occur during a training session. As a result, the body must heal and reinforce the muscles beyond their previous capabilities in order to prepare for the next workout. So technically, this soreness is not a “bad thing” for runners. In fact, it means the training program is likely making you a stronger, faster athlete. If your runner’s aches are truly due to DOMS, the soreness should resolve within three days. It should not limit your ability to go on a recovery run, cross-train, or even perform normal tasks around your home. Proper hydration, nutrition, sleep, and other active recovery strategies, like foam rolling or stretching, will also reduce the symptoms of DOMS.
Check out Impact’s YouTube channel for some post-workout recovery ideas to combat DOMS
Pain
According to the World Health Organization, pain is “an unpleasant sensory and emotional experience associated with actual or potential tissue damage.” Pain occurs as a protective mechanism when the body is injured or thinks it is in danger of injury. So, pain is not always a direct measure of the body’s physical status. Also, this protective response varies among individuals due to differences in genetics, past experiences with pain, and cultural interpretations of pain. These complexities explain why one runner may describe an ache as painful while another runner does not. In order to understand the message that pain is trying to send you, Chris Johnson, a professional runner and physical therapist from the Pacific Northwest, has some things for you to consider:
Chris Johnson Pain Monitoring Model:
Use the scale to assess your “pain” while running as well as in the 24 hours after your run. Then follow the recommended response:
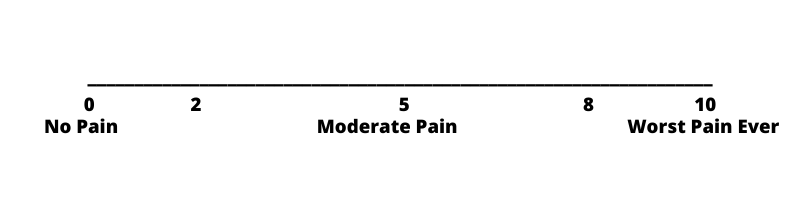
“Safe Pain”
Pain level of 0-2/10 (Pain/symptom is mild and tolerable)
- Continue your current training program with the symptoms.
“Acceptable Pain”
Pain level of 2-5/10 (Pain/symptom is distressing and becoming intense)
- Pain does not go above a 5/10 during the run
- Pain does not go above a 5/10 immediately after the run
- Pain does not go above a 5/10 the morning after the run
- Continue your current training program with the symptoms as long as:
- Do not advance your training until the pain is tolerable for you (< 2 on scale)
“High Risk Pain”
Pain level of >5/10 (Pain/symptom is intense and becoming severe)
- Stop your training and consult with a physical therapist for further evaluation and instruction.
Other Rules to Follow from Chris Johnson:
- Pain and stiffness should NOT increase from week to week of training.
- Regardless of pain level, training should NOT cause altered mechanics while running or while walking afterward.
- Regardless of pain level, training should NOT cause you to use over-the-counter medications for pain relief (Ibuprofen, Tylenol, NSAIDs, etc.).
If you experience any of these above situations, stop your training and consult with a physical therapist for further evaluation and instruction.
By following these guidelines, you can better decipher between the general “aches and pains” of running and the potential onset of a running-related injury. If you have further questions or are confused by any of these recommendations, please reach out to one of our physical therapists. Impact Physical Therapy’s team can help you heal from a previous injury, prevent future ones, and even help optimize your running performance to reach your goals!

